This report as part of that advocacy strategy, highlights some of the laws and decrees in Uganda that infringe on civic freedoms in a bid to rebuild Civic Space in the country. The research reconstructs the various legal processes in the country, portraying what has been changed and what is yet to be changed.
It is worth noting that at least a volume of laws has gradually reduced civil society's freedom of action in Uganda, much as some have been nulled.
One of the specific objectives of this project is to document, analyze and disseminate the impact of laws and policies directly affecting civic space to support advocacy efforts. The research outlined in this report is an integral part of that effort.
The conclusions are based primarily on the real-life experiences and perceptions of the respondents, including human rights defenders and civil society actors involved in the
assessment process. This indicator is based on quantitative data collected during the study.
The State of Disaster could be lifted next week, according to Cooperative Governance Minister Nkosazana Dlamini Zuma, but it’s unclear whether the new draft regulations will replace the previously released proposals or complement them.
he government wants to lift the State of Disaster by 5 April following the gazetting of new regulations aimed at guiding the country’s ongoing response to the Covid-19 pandemic, Cooperative Governance and Traditional Affairs Minister Nkosazana Dlamini Zuma announced in a press conference on Tuesday.
President Cyril Ramaphosa’s Cabinet has been under significant pressure from business groups, opposition parties and healthcare experts to lift the two-year State of Disaster, which has been criticised as a burden on the country’s economic recovery and unnecessary in ongoing efforts to prevent hospitalisations and deaths.
Ramaphosa last week announced his intention to end the State of Disaster around 16 April, after the one month available for public comments on proposed amendments to the National Health Act closed.
On Tuesday, Dlamini Zuma said new draft regulations would be released to manage the response to Covid-19 once the State of Disaster is lifted. They had not been released at the time of writing.
The minister said the public could submit comments on the new regulations for 48 hours, after which the comments would be analysed and, the government hopes, the State of Disaster could be lifted.
It’s unclear whether the new draft regulations will replace the previously released proposals or complement them. Dlamini Zuma’s spokesperson, Lungi Mtshali, did not respond to a request for comment.
It’s also unclear how the government plans to move forward with such a narrow window for public comments on the new regulations while a month was allotted for public comments on the proposals under the National Health Act.
The minister said the new regulations, which would be gazetted and released on Tuesday, made provision for the wearing of masks in indoor public spaces, limitations on gatherings, physical distancing requirements and rules for travellers coming to South Africa.
Ramaphosa outlined the same regulations during his speech last week. He emphasised that the end of the State of Disaster did not signal an end to the fight against Covid-19, suggesting some form of regulations would stay in place in the near future. Dlamini Zuma, however, said the regulations would only last 30 days after they were introduced.
“Though the pandemic is not yet over, it was the desire of government for the country, as much as it is possible, to return to normality, but in a manner that recognises the changing nature of the pandemic,” said Dlamini Zuma.
She defended the State of Disaster, which has been repeatedly extended. “If you look at how we have done through the two years and look at how other countries also have done and compare what happened here now and what happened during the Spanish flu, I think, yes, it was necessary because I think we would have experienced many more deaths if we hadn’t [imposed the State of Disaster].”
Cilliers Brink from the DA welcomed the government’s “climbdown” but remained cautious about future regulations.
“We are deeply concerned that this is only a tactical concession, and that the government intends to hang on to lockdown powers by using national health regulations,” said Brink.
The DA had filed court papers to challenge the extension of the State of Disaster. The trade union Solidarity had also approached the courts and its case is due to be heard on 5 April, the same day Dlamini Zuma said she hopes the State of Disaster is lifted.
Other political parties were also critical. Speaking on the SABC, Cope’s Dennis Bloem said the minister’s press conference was unnecessary and a waste of time.
The IFP’s Mkhuleko Hlengwa said Dlamini Zuma’s address was a “tautology” of Ramaphosa’s earlier address and that the proposed regulations mean “more or less the same, whether it is under a State of Disaster or not”.
UDM leader Bantu Holomisa tweeted: “This is rubbish, it’s creating a permanent State of Disaster scenario. All they’ve done is transfer provisions in the disaster of management act into the Health Act!”
The new Covid-19 regulations published under the National Health Act have been criticised as an attempt by the government to maintain the wide powers it received under the State of Disaster. They allow authorities to impose curfews, mask mandates and limit the distribution and consumption of alcohol. They also introduce new self-isolation and quarantine regulations, which have been criticised as incoherent and illogical.
Source - DM
The solidarity of the human family is fracturing.
We see it all around us. We see it in the comprehensively inadequate efforts by many rich countries to tackle the climate crisis. We see it in the failed response to the crippling debt crisis faced by the world’s poorest countries.
But the pandemic has shown us that countries – especially those from the Asian continent and across the Global South – can powerfully unite in common cause for the betterment of all of humanity.
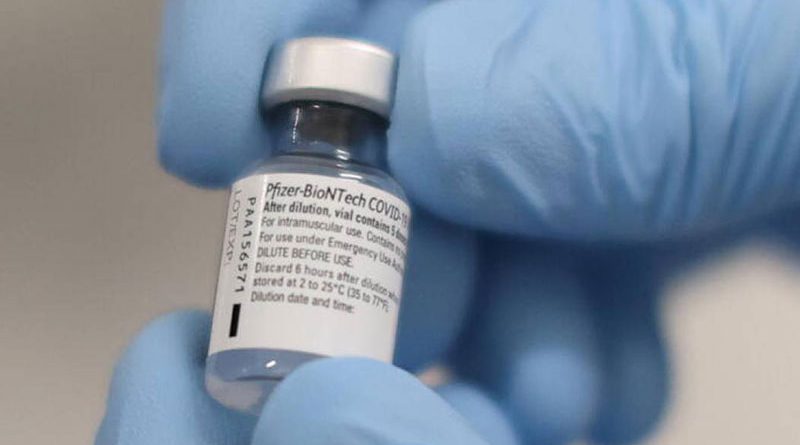
India and South Africa have courageously led a group of over a hundred nations, demanding the rights to manufacture Covid-19 vaccines and treatments, at the World Trade Organization (WTO). By doing so, India and South Africa have asserted that there is something profoundly wrong about a handful of rich nations and their pharmaceutical companies such as Pfizer and Moderna getting to decide who lives and who dies across the world. They, too, have asserted that developing countries must not be a second-class partner in global affairs: but be able to take control of their own destiny.
Significant progress has been made in 18 months. Some advanced economies such as the US and Australia also came on board, agreeing in principle, recognising that extreme vaccine inequity is bad for the world.
But now all that progress is being put to the test, in decisions that will be taken in the next few days.
The European Union (EU) has been the world’s “biggest roadblock“, as former Irish president Mary Robinson described, to the developing world’s efforts to agree a suspension of intellectual property rules on COVID-19 vaccines and technologies at the WTO.
For two years, the EU has actively protected the hyper-profitable pharmaceutical monopolies held over COVID-19 vaccines technologies – even while over a hundred capable manufacturers could have been making them. The global public health leader and executive director of UNAIDS Winnie Byanyima has argued that had such steps been taken, we may have ended the pandemic by now.
But finally, after huge pressure from countries and people around the world, the EU is at the table. It says it is ready to compromise. It has put this to South Africa and India and other countries. Sadly, it is far from an adequate compromise. This is not a TRIPS waiver. After millions of avoidable deaths from COVID-19 and with infections rates soaring once again across our continent, agreeing to it would indeed not be a genuine compromise, but instead a gift for the EU and their pharmaceutical corporations.
There are some positives. The fact that the EU is finally recognising, after nearly two years, that pharmaceutical monopolies are a problem is a step forward. Moreover, the EU driven proposal allows for a partial waiver of restrictions on vaccine exports for generic manufacturers.
But the barriers that remain are inexcusably enormous and, if the objective is to increase and diversify vaccine manufacturing, the EU has failed to deliver. Most fundamentally, the EU-led compromise still denies developing countries and manufacturers essential information necessary to make COVID-19 vaccines. This includes manufacturing know-how, equipment, ingredients, and other information locked up as trade secrets, other forms of intellectual property and other fortresses of commercial confidentiality.
The so-called compromise only relates to vaccines despite desperate and extreme inequality in access to COVID-19 tests and treatments that could be saving lives now, especially in countries where the vaccines are not. And, inexplicably in the midst of a global health crisis, much of the world would be locked out of the agreement, including countries exporting more than 10% of the global vaccine supply, but also, as things stand, the poorest countries and non WTO members.
Perhaps most shameful of all is that far from lifting barriers, the EU has added more.
These include an onerous and nigh on impossible requirement to identify and list all patents related to a vaccine. With 280 components for the mRNA vaccines alone the patent landscape can be incredibly complex and contested; much of the information required may not even be in the public domain. Importantly for India, such patent listing is not a requirement of Indian law and endorsing it would therefore constitute a retrograde step for the nation.
We recognise some seeds of progress here. But the shallowness of this compromise is deadly.
After an estimated 20 million lives have been lost to COVID-19, at a time in which COVID-19 has killed four times more people in the poorest countries than rich countries, we must ask: is this really the best that the rich world can offer?
Source : The WIRE